Human diseases come and go. When I was young, in the 1950s, children were threatened by polio (also called infantile paralysis). That concern was erased by the Salk vaccine, and later the Sabin vaccine. In the mid-70s, the smallpox virus was actually eradicated from the earth (apart from a few samples kept in highly secured laboratories), which was possible only because the disease is carried only by humans, and has no animal vector. But there are now new diseases that were not threats when I was young. AIDS (Acquired Immune Deficiency Syndrome) didn't exist in my youth, for example. My children and their neighborhood friends routinely played outdoors on warm summer evenings, without a care in the world. But mosquitoes in Massachusetts now carry West Nile disease, and sometimes Eastern Equine Encephalitis, both of which can be fatal. And ticks, which are easily picked up in our wooded yard, now carry Lyme disease, and other diseases as well, which brings us to Ixodes scapularis. I don't know what it was that moved north from Old Lyme, Connecticut, where Lyme disease was first detected and named. Was it the ticks? Or were the ticks always there, and only the infection moved north? Whatever the case, Lyme disease is an ongoing concern for us. In the summer, we need to routinely check our bodies for ticks, preferably every day. We find them quite often. I must at this point issue a disclaimer: I am not a doctor, and nothing in what follows should be taken by anyone as medical advice. Consult your own personal physician on these issues. This is merely the story of some of our interactions with Ixodes scapularis, as I remember them. Let me begin by introducing Dr. Leonard Marcus. He was not my primary physician, nor was he Margie's. He was originally referred to us for a telephone consultation about travel, when our older daughter Elissa was thinking about taking a semester abroad from Brown University. She started by asking for a comparison between the medical hazards of travel in Madagascar vs. Australia. Dr. Marcus discussed the various tropical diseases that might be a problem in Madagascar, including the necessity for prophylaxis against malaria. He also noted that the medical system in Madagascar is not the best, but the island doesn't have very many poisonous animals. Australia, on the other hand, has the largest number of toxic animals of any country on the face of the earth, in both the land and the sea. This includes snakes, spiders, and jellyfish, among others. While Australia has an excellent medical system, that might not do you much good if you're stung or bitten far out in the bush. That conversation was our introduction to Dr. Marcus, and we continued to consult him whenever any member of our family traveled to developing countries. Since our two daughters between them did a lot of travel, often in the third world, we consulted him often. Our daughters, between them, traveled to Botswana, Grenada (West Indies), India, Kenya, Madagascar, Mali, Mozambique, Nepal, Pakistan, South Africa, Thailand, Uganda, Western Samoa, and Zimbabwe, not to mention a host of countries in South America, Central America, and Europe which were tame by comparison. Our daughters didn't always like his lectures, in which he drilled them on precautions they needed to take when traveling in the third world. These included avoiding the local water (which might be disguised as ice), avoiding food from unknown sources such as market stands, eating primarily cooked food, and so on. Dr. Marcus suggested that Elissa be tested shortly after returning from Madagascar, to see if she'd picked up anything that wasn't evident. And indeed, she initially showed an antibody reaction to schistosomiasis (snail fever, a very dangerous disease), indicating that she had been exposed to it. However, subsequent testing showed that she had not acquired the infection. Dr. Marcus also advised us on two separate occasions when, coincidentally, each of our daughters was nipped by a stray dog in Costa Rica (not the same dog, obviously). This had happened despite each of them carefully attempting to follow his advice to never interact with stray animals. Oddly, both Elissa and Sara had previously received pre-exposure rabies inoculations, Elissa for her travels in Madagascar, and Sara for travel on the Indian subcontinent. Still, Dr. Marcus recommended that they each receive a couple of rabies booster shots. When one has had the preexposure inoculations, these are pretty simple, and rabies is a universally fatal disease not to be taken lightly. Sara's employer once sent her, with one day's notice, from Cape Town, South Africa to Karachi, Pakistan (he did things like that). Cape Town had no malaria risk, whereas Karachi had a slight risk of a chloroquine-resistant malarial strain. The short notice meant that Sara didn't have time to start the necessary anti-malarial Lariam the requisite one week in advance of travel to a malarial area. Sara phoned Dr. Marcus from Cape Town to discuss the issue, and he spent quite a bit of time explaining the risks of starting the medication late, and the side-effects of Lariam. Sara did make the trip, and didn't start the Lariam until arrival, to avoid any possibility of experiencing some of its more serious side-effects while in transit. In addition to being an infectious disease specialist, Dr. Marcus was also a parasitologist, which finally brings me back to Ixodes scapularis. Upon finding a tiny deer tick attached to my body one day, I plucked it off with tweezers. Not knowing what to do with it, I stuck it to a piece of tape, and took it off for Dr. Marcus to see. He was annoyed that I had stuck it to the tape, which mangled its body a bit, and made it difficult for him to identify under his microscope. Nevertheless, he was fairly confident that it was a deer tick, Ixodes scapularis, putting me at risk for Lyme disease. Over the years, Margie and I have found quite a few of these deer ticks, and I gradually learned from Dr. Marcus what I need to observe about them. He taught me the lifecycle of the deer tick, which has four phases: egg, larva, nymph, and adult. In each stage beyond the egg stage, the tick must eat a blood meal (the larva and nymph, to be able to pass to the next stage, and the adult to be able to lay eggs). These meals are typically obtained from a deer or a mouse, but can be gotten from any mammal, including humans. But if the tick picks up a disease organism from its host in one stage, it can pass that disease on to its next host when it bites in the subsequent stage. Curiously, when it bites, the tick doesn't pass the disease on immediately. It spends a certain amount of time injecting anticoagulants and numbing agents so it will not be detected by the host. Only when starts sucking significant amounts of blood can it transmit the disease-causing organism. Thus a tick needs to be attached for some amount of time, perhaps 24 to 36 hours, before there's any risk of the disease having been transmitted. Dr. Marcus was happy to explain all of this to me. As a result, I learned that it's important to identify the tick, its stage of life, and whether or not its body is engorged with your blood (which is pretty clearly visible).
But it's not engorged - its belly is not blown up, and I believe it to have been biting me for less than 12 hours. This means I was not at risk of transmission of disease. Hence I took no action, other than picking it off and sending it to its doom in a vial of alcohol (as Dr. Marcus taught me).
This required treatment with the antibiotic doxycycline. But because the tick had not been on long (it was just beginning to get engorged, and had not yet completed its feeding and dropped off), a single treatment was deemed sufficient. Sometimes treatment is followed up with a test for the Lyme organism a bit later, to be sure that the treatment was long enough, and an infection has been avoided. On another occasion when I brought Dr. Marcus a tick, he got very excited when he put it under his microscope. He called me over, had me look at it through the microscope, and asked me what I saw. Not being as discriminating as he, all I could say was, "I see a tick." "Count the legs", he said. I counted. There were six of them. Only six legs; Dr. Marcus explained that this meant that I had brought him a larva, the earliest stage of the tick's life after hatching from an egg (the nymph and adult stages have eight legs). I was the first host this tick had ever bitten. Thus I was completely safe. Never having previously bitten anything else, it had not had a chance to pick up any diseases. The reason Dr. Marcus had been so excited was because I was the first person to ever bring him a larval deer tick. They are so tiny that victims of their bites seldom find them at all. I've been showing you blown up pictures of ticks taken with my camera in macro mode. Some of my readers with dogs may be thinking these are similar to dog ticks, which are often half a centimeter long (0.2 inches), and even larger when engorged. This is not the case; even in its nymph and adult stages, Ixodes scapularis is tiny. The picture below shows the tick two pictures above (the one that's not engorged) on the tip of my finger; it's less than a millimeter long. And I spotted it sucking on my ankle - but remember, I was sharp-eyed enough to have once spotted a larva. 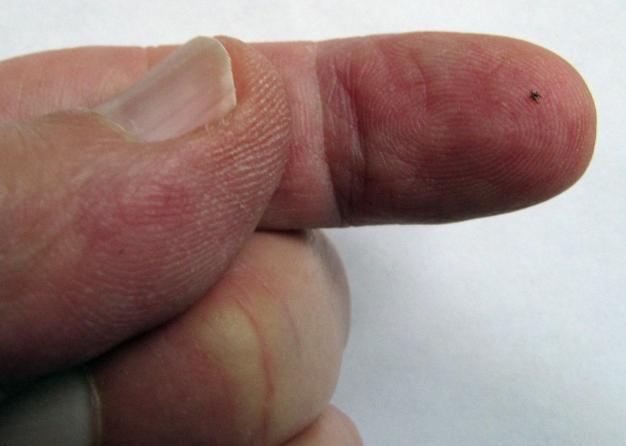
Both Margie and I have needed these treatments at one point. We were treated with doxycycline for either three weeks or five weeks, but the course of treatment apparently now been reduced to only two weeks. For a long time, the recommendations of the CDC (the Centers for Disease Control in Atlanta, Georgia) were to not treat until a rash showed up. This struck me as a rather bad idea, because it's known that a rash doesn't show up in every case. Thus, someone bitten by a tick might think he or she was in the clear, when in fact an infection had been passed on. The trouble was, most doctors didn't seem to be capable of doing what Dr. Marcus did. They couldn't identify the tick, distinguish its stage, and tell whether or not it was engorged. We were thus not very happy a number of years ago when Dr. Marcus retired, and we could no longer consult him about our tick bites. But the medical profession in this area seems to have now seen Lyme disease so frequently that they've started to catch up with Dr. Marcus. Most doctors in the area now will examine ticks, and treat the tick bite even if a rash does not appear.
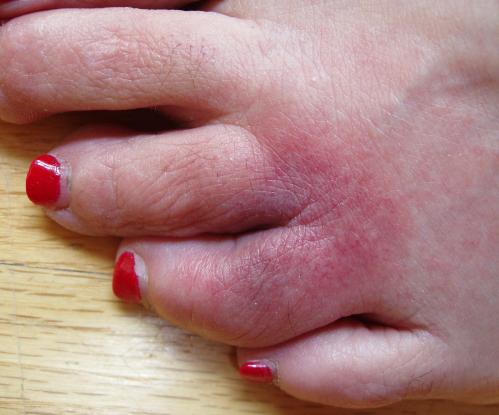
What was this? It didn't seem like the characteristic bull's-eye rash of a Lyme infected tick bite, but then again, bull's-eyes normally form on flat areas of skin. Could this be the form the rash takes on toes? Margie was not aware of having been bitten by a tick, but then it could have easily hidden between the toes (the photo shows the rash in its early stages - it actually spread more widely). There was also another possible diagnosis, a condition called cellulitis. And cellulitis can quickly blossom into an extremely dangerous condition. In that sense, it was more of a concern than Lyme disease, since Lyme disease in that early rash stage could be treated. A test for Lyme was done, but such tests are often negative if done too early. Margie's doctor decided to simply treat with doxycycline, a low risk treatment which would cure the Lyme disease (if that's what it was). This was based on her clinician's judgment that Lyme disease, given the appearance of the rash, was a more likely scenario. And indeed, the rash cleared up within a day after the doxycycline was started. All of this concern might seem to some of my readers unfamiliar with Lyme disease to be a bit overblown. But it's not, because it's extremely important to catch this disease early on. If you stop it immediately after the tick bite, only a single dose of doxycycline is required. If you don't catch it until the rash appears, it takes a couple of weeks of treatment, but it's still entirely curable. But if you miss it in these early stages, then you can be in trouble. It can produce serious symptoms that can go on for years. It's uncertain whether the disease itself becomes chronic, or whether the infection clears up but leaves long-lasting after-effects, or even if some of the serious symptoms reported as Lyme disease are due to other diseases carried by the same ticks. A recent article in the New Yorker discussed various theories about this subject, and another recent article in the Boston Globe notes that there are four other infections carried by the same ticks, and it's hard to sort out what problems are caused by what disease organisms. But it's quite clear that you want to catch and treat these tick bites as early as possible. This little dot, about the size of a poppy seed, can cause an awful lot of trouble. Will my granddaughter be able to play in our yard like my daughters did? Curse you, Ixodes scapularis!
  |

 To the right, you can see a picture of a tick that I recently picked off my body. Its legs are curled due to the bath I gave it in isopropyl alcohol. I believe it to be a nymph, but it could possibly be an adult (Dr. Marcus would know, but I'm not that good at it).
To the right, you can see a picture of a tick that I recently picked off my body. Its legs are curled due to the bath I gave it in isopropyl alcohol. I believe it to be a nymph, but it could possibly be an adult (Dr. Marcus would know, but I'm not that good at it).
 For comparison, the picture on the left shows a tick which we recently found munching on Margie. You can see that its rear end is blown up, and light in color. This is a tick that's engorged, meaning that Margie somehow must have missed it for a day.
For comparison, the picture on the left shows a tick which we recently found munching on Margie. You can see that its rear end is blown up, and light in color. This is a tick that's engorged, meaning that Margie somehow must have missed it for a day.
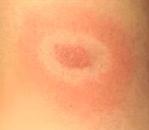 Their tiny size is why they're so easy to miss, in which case you don't know you've been infected with Lyme disease until the characteristic rash appears a bit later. This is often a "bull's-eye" rash, like the one shown to the right. But if you don't treat with antibiotics until the rash shows up, a longer course of treatment is required.
Their tiny size is why they're so easy to miss, in which case you don't know you've been infected with Lyme disease until the characteristic rash appears a bit later. This is often a "bull's-eye" rash, like the one shown to the right. But if you don't treat with antibiotics until the rash shows up, a longer course of treatment is required.